Clinical trials are research studies in which patients volunteer to help find answers to specific questions, typically with regard to new treatments. In prostate cancer over the last decade, the majority of clinical trials have been in the advanced prostate cancer setting. This has resulted in many new, effective treatment options for these men. This article will introduce you to the basics of “what is a clinical trial?”
What is a clinical trial?
Clinical trials are part of clinical research and at the cornerstone of medical advancement. The goal of a clinical trial is to determine if a treatment or intervention is safe and effective. These trials are conducted according to a trial protocol (i.e., a plan), which describes several key elements of the clinical trial:
- The types of patients that are eligible for trial enrollment
- The timing, or schedule, of tests and/or procedures that are involved in the trial
- The drugs or intervention that is involved in the trial
- The dose or amount of drug to be given in the trial
- Safety assessments that will be included during the follow-up period
- What the doctors or researchers hope to learn from the trial
Before enrolling in a clinical trial, potential patients are screened for eligibility for the trial. This is done for several reasons. The first reason is to ensure that the patients enrolled are the type of patients that will be best suited for answering the clinical question outlined in the clinical trial protocol. The second reason is to ensure that patients are healthy enough to be in the trial and will not be subject to undue harm. One of the most basic clinical trial designs used in prostate cancer is randomizing patients (usually 1 to 1) to receive either the current best clinical care (termed the standard of care, the control group) versus a new treatment (intervention group). The treatment or intervention group may include treatments that are currently part of the best available clinical care. All of these patients are then followed the exact same way to evaluate if they develop the primary outcome as defined by the trial protocol:
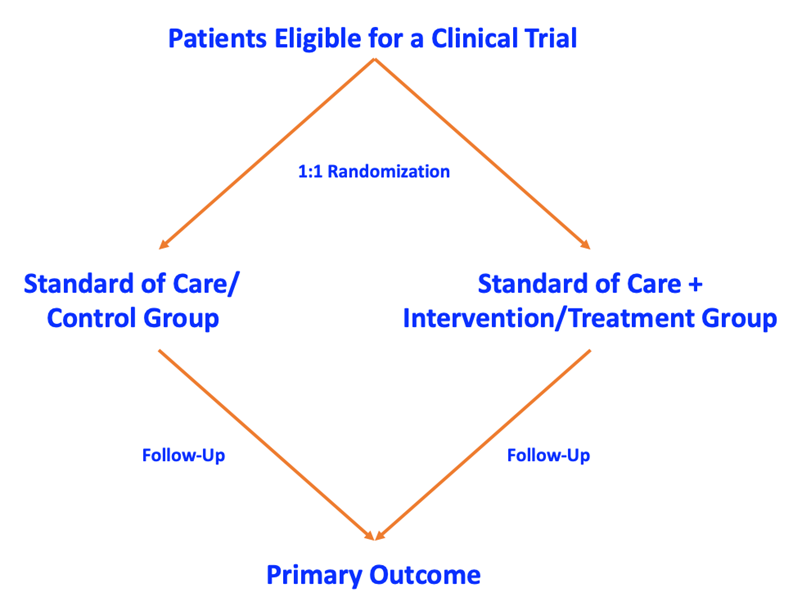
Let’s look at a real-world example of advanced prostate cancer. The ARASENS trial recruited men with metastatic hormone-sensitive prostate cancer (mHSPC) and randomized them to either standard of care (ADT + docetaxel) versus the standard of care + new treatment (ADT + docetaxel + darolutamide). Put simply, this trial was assessing if the addition of darolutamide to the standard of care improved outcomes in men with mHSPC compared to standard of care alone. The primary outcome for this study was predetermined at the time of trial design to be overall survival:
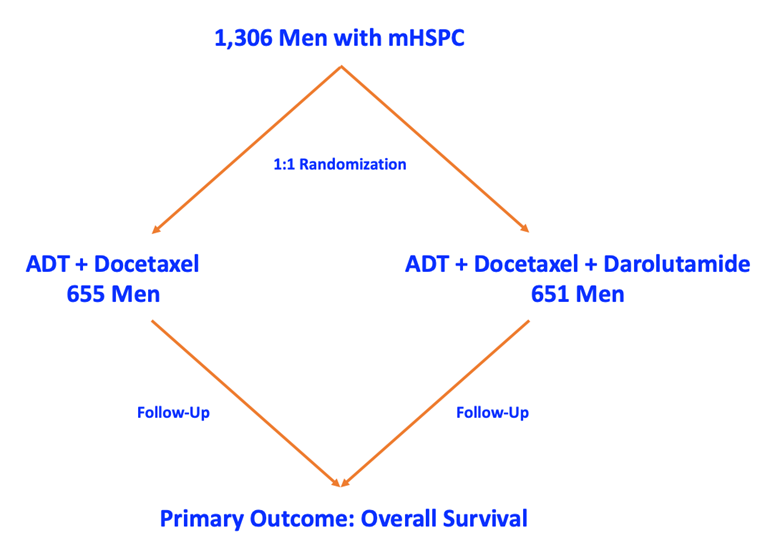
The ARASENS trial showed that the risk of death was significantly lower, by 32.5% (hazard ratio 0.68, 95% confidence interval 0.57 to 0.80), in the darolutamide group (the intervention) than in the patients who did not receive darolutamide (the control group). Thus, because of men willing to enroll in this clinical trial, a well-designed and executed protocol, and a statistically significant primary outcome (overall survival), the addition of darolutamide to ADT + docetaxel was given FDA approval for the treatment of men with mHSPC in August 2022.
It is important to understand that volunteers in the clinical trial must agree to the rules and terms outlined in the protocol. Similarly, doctors and researchers who manage clinical trials must adhere to the clinical trial protocol and the rules set out by the U.S. Food and Drug Administration (FDA), to ensure that clinical trials are ethical, safe, and advancing the field of prostate cancer. As mentioned, a clinical trial entry is entirely voluntary. If you decide to not enroll in a clinical trial, your doctors will continue to treat your prostate cancer with the best standard of care available.

